The NHS always talks about patient participation. I don’t think that someone who is on the verge of ending their life would be asked to rate on a scale of one to ten if they feel listened to by their social worker – but the intention is clear – those receiving the mental health services should be involved in designing and assessing the care that they receive. My mother-in-law, Karen Ross, MBE, told me that she always thought that to be ill you need to be well. And she is right. I have a lot of experience of being within the mental health system but when I was ill (in that way) I just didn’t have the strength to try and understand the health system, to chase medical appointments and also to get angry – but articulate – when the system wasn’t working for me. But now I am not feeling so depressed (just cognitively inept) and in the spirit of patient participation, I present to you my own mental health manifesto, part one – the cheap one (part two tomorrow is expensive).
When a patient first visits a GP saying they are depressed they should be given two information sheets – one would have a simple organisational flow chart to explain how the mental health system works in their area and another would detail non-NHS resources that they could turn to, in case, as is 100% likely, their referral doesn’t come through as quickly as they would like.
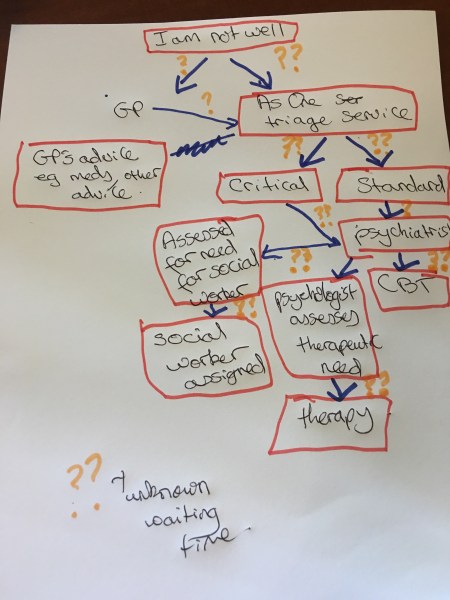
- Organisational flow chart –
After three years in the Hertfordshire Partnership University NHS Foundation (ie the Mental Health Trust) system I am now going to try and explain to you the steps a patient has to take on their mental health journey (although some management consultant is probably plotting to change the system as we speak). Firstly you have trot off to your GP you say ‘I am depressed’ and if the doc thinks you need more than a tablet s/he will refer you to the As One services. You can also decide to just skip that bit and phone up As One yourselves. As One then make an appointment with you for a short triage session at their specialist centre (ie a call centre). For those of you that don’t know, there are a hell of a lot of depressed people out there today, and even feeling suicidal is not enough to get you mental health care quickly. You need to feel that you are going to do the deed in the next ten minutes if you want immediate help. If you only have the S thought once a week the call centre (maned, it has to be said, by trained therapists and the like) put to the back of the queue. The call centre then assigns you to one of two services – what I call the Critical or Standard service. If you are assigned to the Critical Service, about six weeks after going to the GP telling him/ her that you desperately wanting to kill yourself you can finally see a psychiatrist. You tell them your woes and s/he gives you a tablet and also gives you a nice label eg bipolar, borderline personality disorder, generalised anxiety disorder etc. Sometime after that you might get an appointment to see a clinical psychologist who tells you what type of therapy s/her thinks is best for you (but she won’t be able to tell you what the waiting time to see a therapist is like). And eventually after all these shenanigans you are put on a list to see a therapist. In between all of this you might also be given a social worker to perk you up every now and then. So are you with me? That’s six people (and it could be more) that you have to tell your life story to if you are feeling shit. I think, it’s much better to be a patient in the Standard group because then you have to wait a bit longer to see a psychiatrist but you are just assigned a Cognitive Behavioural Therapist and you can relax a bit and feel less confused. Don’t get me wrong, most of people that work in the Service are extremely helpful, caring and work very hard in a particular stressful situation. But I am sure you will agree with me that an organisational flow chart of how the system works would be useful for each patient, preferably with target wait times for each appointment.
NB – If you think that no-one should have to explain their inner soul to seven different people when you are depressed, then I agree with you. This will take a lot of extra funding and I will discuss this tomorrow.
- The second sheet of paper would have a list of four different types of non- NHS resources that are available to so that patients can be signposted to what can literally be life-saving resources if, as is inevitable their referral takes longer than is expected.
- i) Specialist mental health charities
We are blessed in this country to have many mental health charities that can provide excellent support eg Mind (there’s one in Leeming Road, Borehamwood), the Jewish Association of Mental Illness (JAMI) and many others. GPs should be fully informed about these services and signpost patients to them if it’s appropriate.
- ii) Online support groups.
The NHS has an excellent support portal for people suffering with mental health issues – called the BigWhiteWall – but GPs need to be aware of it and advocate for its ability to show patients that they are not alone and that other going through similar troubles can help them. Facebook also has an array of specialist support groups.
iii) Mindfulness resources.
If you read the literature on mindfulness it says that, if practiced regularly, mindfulness can help you find true inner peace and joy. It might not achieve all of your expectations but it can help. There are lots of mindfulness apps on the internet (free or paid for) as well as face to face groups – and patients should be given details of them when they first go to their GP (Personally I think that the NHS should have its own free mindfulness app for patients but that’s a different story).
- iv) Paid for services
It isn’t really controversial to admit that some people pay for services when they know that the NHS isn’t meeting their expectations. And therefore I think that on this piece of paper should be a list of paid-for mental health services eg registered private therapists listed on the British Association for Counselling and Psychotherapy or the UK Council for Psychotherapists search facility.
So that is the first part of my mental health manifesto. When a patient comes to see a GP – give them two pieces of paper (or to cut costs one double sided-piece of paper). Tomorrow – part two.